Bronchiolitis Obliterans : Complete Guide - Causes, Symptoms, Diagnosis and Treatments
Published on March 9, 2026 by Johann
Relative of someone with BO
Also known as: popcorn lung · constrictive bronchiolitis · PIBO · BOS · popcorn lung
Updated on March 9, 2026 — Sources: NCBI, PubMed, Orphanet, ERS/ATS/ISHLT, Frontiers in Pediatrics, RespiRare
Summary
- In summary: what is bronchiolitis obliterans?
- Medical definition
- Causes and risk factors
- Pathophysiology: what happens in the lungs
- Symptoms: how the disease manifests itself
- Diagnosis: how to confirm the disease
- Severity classification (post-transplant BOS)
- Treatments: current therapeutic options
- Prognosis and progression
- Prevention: how to reduce risks
- Research prospects and recent advances
- Frequently asked questions (FAQ)
In summary: what is bronchiolitis obliterans?
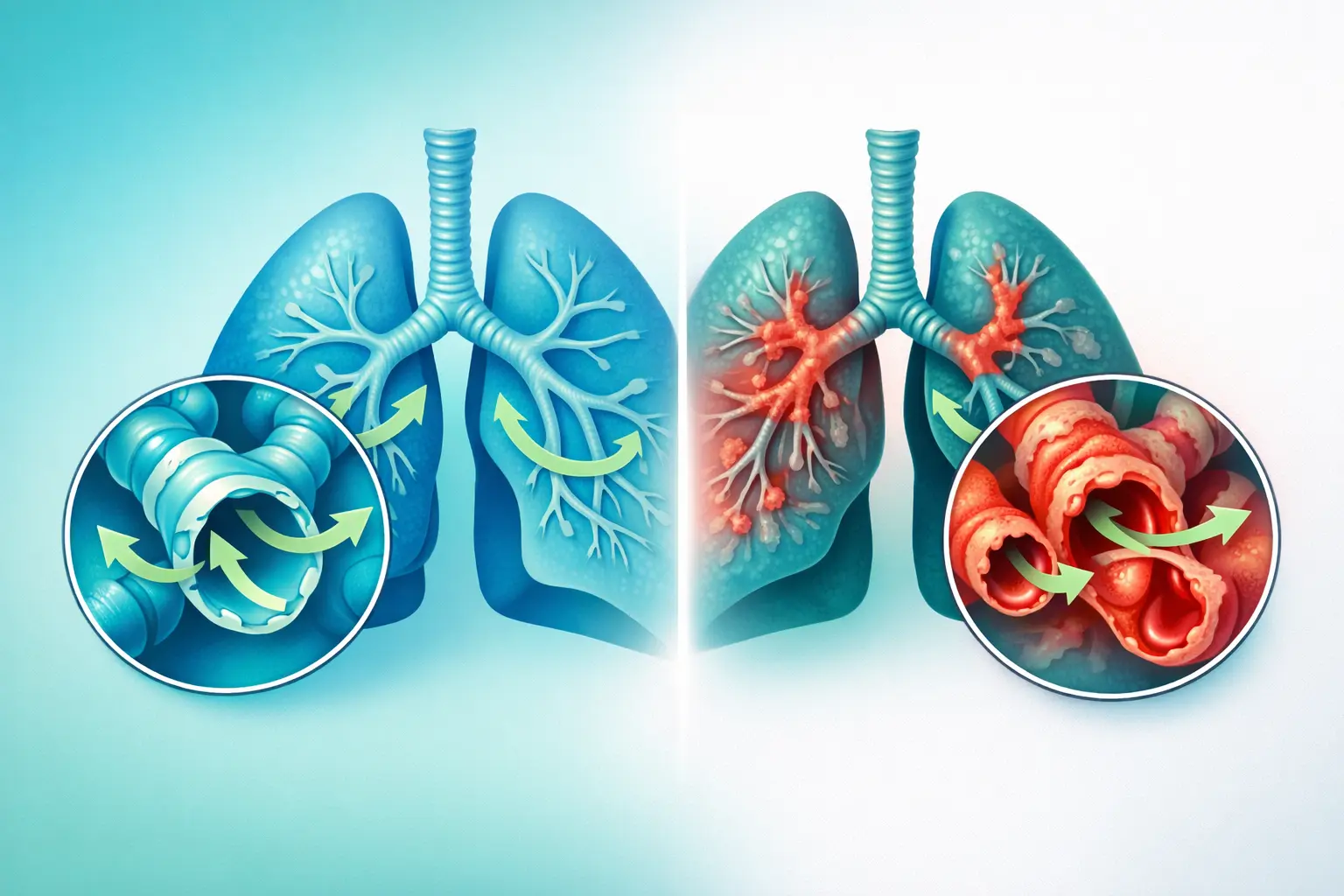
To understand it simply: imagine your lungs as a tree. The large branches are the bronchi, and at the very end, there are thousands of tiny twigs: these are the bronchioles . Bronchiolitis obliterans is when these small twigs become inflamed, scarred, and gradually blocked. It becomes increasingly difficult for air to circulate. You find it harder to breathe, you cough, and you tire quickly. Unfortunately, this damage is usually irreversible .
It is a rare, chronic, and serious disease. It can affect both children and adults, but for very different reasons. In children, it most often occurs after a major respiratory infection (known as post-infectious bronchiolitis obliterans). In adults, it is frequently linked to organ transplants (lung or bone marrow), inhalation of toxic substances, or certain autoimmune diseases.
The nickname "popcorn lung" comes from a striking story: in the early 2000s, in the United States, popcorn factory workers developed this disease after years of inhaling a chemical, diacetyl, which gave popcorn its buttery taste. Today, this link has also been suggested in relation to certain e-cigarette flavors, although no cases of bronchiolitis obliterans directly linked to vaping have been confirmed to date in individual consumers.
In other words, this is not the classic bronchiolitis seen in infants (which is acute and viral), but a chronic and much more serious lung disease.
Medical definition of bronchiolitis obliterans
Bronchiolitis obliterans (BO), also known as constrictive bronchiolitis or chronic bronchiolitis obliterans, is an obstructive lung disease characterized by transmural and circumferential inflammation of the terminal and respiratory bronchioles. This inflammation progresses to peribronchiolar fibrosis with progressive narrowing—or even complete obliteration—of the small airways, while sparing the alveolar spaces and distal lung parenchyma.
Classified as a rare disease by Orphanet (code ORPHA:1303), BO was first described under this term by Reynaud in 1835 and clearly characterized in the scientific literature from 1981 onwards. Its exact incidence in the general population remains difficult to establish, but it affects a significant proportion of transplant patients: approximately 75% of lung transplant recipients at 10 years, and between 5% and 14% of hematopoietic stem cell transplant recipients.
Be careful with terminology: bronchiolitis obliterans (BO) should not be confused with bronchiolitis obliterans with organizing pneumonia (BOOP), now called cryptogenic organizing pneumonia (COP) . These are two distinct clinical and histological entities. BOOP/COP affects the alveoli in addition to the bronchioles and generally responds well to corticosteroids, while BO is strictly a bronchiolar disease that is often refractory to treatment.
Causes and risk factors
There are many causes of bronchiolitis obliterans. Four main etiological categories are traditionally distinguished.
1. Post-infectious bronchiolitis obliterans (PIBO)
This is the most common form in children. It occurs after a severe respiratory infection that damages the bronchiolar epithelium, triggering an inflammatory and then fibrotic response leading to obstruction of the small airways.
The main pathogens involved are:
- Adenovirus (serotypes 3, 7, 11, 21, and more recently 55) — responsible for 20 to 69% of POBI cases. Up to 28% of children who survive severe adenovirus pneumonia may develop POBI.
- Mycoplasma pneumoniae — increasingly implicated, especially in older children, with a growing incidence in Asia.
- Respiratory syncytial virus (RSV), influenza, cytomegalovirus, HIV, HHV-8.
- Bacterial and fungal infections are less common.
Identified risk factors for developing BIP after adenovirus pneumonia include: hypoxemia, persistent wheezing, use of mechanical ventilation, prolonged hospitalization, and duration of fever.
Notably, the diagnosis of BIPO is often significantly delayed. The literature reports an average delay between the onset of symptoms and diagnosis ranging from 15 to 88 months. This delay is due to the similarity of symptoms to uncontrolled asthma.
2. Post-transplant bronchiolitis obliterans syndrome (BOS)
This is the main cause of medium- and long-term lung transplant failure. BOS is considered a form of chronic graft rejection. More than 50% of recipients develop some degree of BO within 5 years, with an average time to diagnosis of 16 to 20 months.
After hematopoietic stem cell transplantation (allogeneic bone marrow transplantation), BO occurs in 5 to 14% of cases and is a manifestation of chronic graft-versus-host disease (GVHD). The risk is estimated at approximately 14% in patients who develop chronic GVHD.
Risk factors include: episodes of acute cellular rejection, the presence of anti-HLA antibodies, gastroesophageal reflux with microaspiration, smoking, and certain viral infections occurring within the first 100 days post-transplant.
3. Toxic or occupational bronchiolitis obliterans
Inhalation of irritating chemicals can cause BO. The most well-documented toxic agents include: diacetyl (butter flavor), sulfur dioxide, nitrogen dioxide (agricultural silos), ammonia, chlorine, thionyl chloride, methyl isocyanate, hydrogen fluoride, phosgene, mustard gas, and ozone.
The emblematic case of diacetyl and "popcorn lung": in the early 2000s, NIOSH documented cases of BO among workers at a popcorn factory in Missouri who were heavily exposed to diacetyl vapors. This compound (C₄H₆O₂), which occurs naturally in butter and cheese, causes chronic inflammation of the bronchioles when inhaled in large quantities over a long period of time.
The link with vaping: in 2015, a Harvard University study detected the presence of diacetyl in certain flavored e-liquids. In 2019, the Canadian Medical Association Journal reported a case in a vaper. However, to date, no series of cases has formally established that vaping causes BO on a population scale. In France and Europe, most manufacturers have removed diacetyl from their products. Nevertheless, caution is still advised: more than 180 flavoring agents used in e-liquids have never been tested for inhalation.
4. Bronchiolitis obliterans associated with autoimmune diseases
Several systemic diseases are associated with the development of BO: rheumatoid arthritis (the most common), systemic lupus erythematosus, inflammatory bowel disease, Stevens-Johnson syndrome, paraneoplastic pemphigus, and more rarely, juvenile idiopathic arthritis or IgA nephropathy.
In rare cases, no etiology can be identified: this is referred to as idiopathic or cryptogenic bronchiolitis obliterans.
Pathophysiology: what happens in the lungs
The pathogenic mechanism of BOB follows a common pattern, regardless of the initial cause, although certain specificities vary depending on the etiology.
Phase 1 — Initial injury: a lesion damages the epithelial cells of the terminal and respiratory bronchioles. This injury may be infectious, chemical, immunological, or ischemic. It causes localized necrosis of the bronchiolar epithelium.
Phase 2 — Dysregulated inflammatory response: inflammation of the subepithelial structures leads to an accumulation of fibrinopurulent exudate in the bronchiolar lumen. Infiltration by lymphocytes, neutrophils, and macrophages is observed. Pro-inflammatory cytokines (IL-8, IFN-γ) are significantly elevated.
Phase 3 — Fibroproliferation: denudation of the mucosa exposes the myofibroblasts of the submucosa, which proliferate excessively. This aberrant repair process leads to the deposition of collagen and acidic mucopolysaccharides, progressively narrowing the bronchiolar lumen.
Phase 4 — Fibrosis and obliteration: fibrous tissue partially or completely fills the lumen of the small airways, causing fixed and irreversible obstruction. Sometimes, intraluminal polyps (Masson's bodies) form through the proliferation of histiocytes and capillaries.
In the context of lung transplantation, the mechanism specifically involves microvascular insufficiency and alloimmune responses directed against the graft.
Histopathologically, there are two types: constrictive (peribronchiolar fibrosis with external compression) and proliferative (intraluminal obstruction by granulation tissue polyps). These two forms can coexist.
Symptoms: how the disease manifests itself
Bronchiolitis obliterans is an insidious disease. Symptoms are often nonspecific at first, which explains the frequent diagnostic errors and delays. They usually appear 2 to 8 weeks after the initial attack and then gradually worsen.
The main symptoms include:
- Progressive dyspnea: initially during exertion (climbing stairs, running), then at rest in advanced forms. This is often the first sign.
- Persistent dry cough: nonproductive, unresponsive to conventional cough or asthma treatments.
- Wheezing: especially when exhaling.
- Chronic fatigue: decreased exercise tolerance.
- Bronchorrhoea: increased bronchial mucus secretion in advanced stages.
- Late hypoxemia: gradual decrease in blood oxygen saturation.
In children in particular: symptoms persist for more than 6 weeks after a severe acute infection, with tachypnea, chronic productive cough, and diffuse crackles on auscultation. Children who were previously healthy do not return to normal respiratory function.
⚠️ Caution — Diagnostic pitfall: BO is often confused with uncontrolled asthma, COPD, or a simple "post-infectious cough." The crucial difference is that bronchial obstruction in BO is fixed and not reversible with bronchodilators, unlike asthma.
Diagnosis: how to confirm the disease
The diagnosis of bronchiolitis obliterans is based on a combination of clinical, functional, and radiological evidence.
Questioning and clinical examination
The doctor looks for a history of exposure (severe infection, recent transplant, occupational exposure), a compatible timeline, and persistent, irreversible symptoms. Auscultation may reveal expiratory wheezing and/or crackles.
Respiratory function tests (RFT)
Spirometry shows an obstructive ventilatory disorder characterized by a decrease in FEV1 (forced expiratory volume in one second), which is not reversible with bronchodilators. The FEV1/FVC ratio is reduced. The 25-75% FEV1 measurement may be altered early on.
High-resolution chest CT scan (HRCT)
This is the key imaging test. Characteristic signs include: a "mosaic" appearance of perfusion, air trapping visible on expiratory slices, thickening of the bronchiolar walls, and sometimes central bronchiectasis.
Bronchoscopy and bronchoalveolar lavage (BAL)
BAL frequently shows elevated neutrophilia (46% to 90% of cells). It also allows active infection to be ruled out.
Lung biopsy
Surgical lung biopsy remains the gold standard for a definitive diagnosis. It shows peribronchiolar inflammation, fibrosis, and obliteration of the lumen. However, it is invasive and prone to sampling errors. International guidelines (ISHLT/ATS/ERS) now allow a diagnosis of BOS to be made on the basis of a decline in FEV1 without biopsy.
Other additional tests
An ECG can be used to look for signs of pulmonary hypertension. Nocturnal oximetry can reveal desaturation. Biological tests can rule out other causes.
Clinical prediction tool (Colom & Teper) for IPBO: a score based on three variables—a typical history of severe bronchiolitis in a previously healthy child, documented exposure to adenovirus, and a mosaic pattern on HRCT—allows for early suspicion of the diagnosis. A score ≥ 7 suggests a high risk of IPBO.
Severity classification (post-transplant BOS)
The ISHLT (International Society for Heart and Lung Transplantation) has defined severity stages based on the percentage decline in FEV1 compared to the best post-transplant value.
| BOS stage | FEV1 relative to best value | Meaning |
|---|---|---|
| BOS 0 | > 90 | Normal |
| BOS 0-p | 81–90% and/or DEM25-75 ≤ 75% | Potential (early warning) |
| BOS 1 | 66–80 | Mild |
| BOS 2 | 51–65 | Moderate |
| BOS 3 | ≤ 50% | Severe |
Each stage is subdivided into "a" (without histological documentation) and "b" (with biopsy confirming BO).
Treatments: current therapeutic options
⛔ Essential information: bronchiolitis obliterans is an irreversible and chronic disease. There is no cure. The therapeutic goal is to slow progression, relieve symptoms, and prevent complications.
Elimination of the causative agent
In cases of occupational toxic exposure, the first step is to immediately stop exposure. After transplantation, optimizing immunosuppression is the priority.
Drug treatments
- Corticosteroids: systemic (prednisone, methylprednisolone) and/or inhaled (fluticasone). IV boluses of methylprednisolone (20-30 mg/kg for 3 consecutive days, repeated monthly for 3 to 6 months) are used in children with PIBO, with clinical improvement in the majority of cases.
- Azithromycin: a macrolide antibiotic with anti-inflammatory and immunomodulatory properties. Standard treatment for post-transplant BOS. As a prophylactic, it reduces the prevalence of BOS. Recent warnings have highlighted a potential risk of excess mortality due to tumor relapse in certain contexts, requiring careful evaluation.
- Immunosuppressants: cyclophosphamide, tacrolimus, cyclosporine—used mainly in autoimmune or post-transplant forms.
- Inhaled bronchodilators: limited efficacy (fixed obstruction), but partial symptomatic relief possible.
- Montelukast: leukotriene antagonist, increasingly used as an adjuvant (FAM triple therapy: fluticasone, azithromycin, montelukast).
- Targeted therapies (prospects): pro-inflammatory cytokine inhibitors are a promising avenue of research.
Non-drug treatments
- Oxygen therapy: at home in cases of chronic hypoxemia, particularly at night or during exertion.
- Pulmonary rehabilitation: structured exercise and therapeutic education programs.
- Extracorporeal photopheresis (ECP): an emerging technique in refractory post-transplant BOS, with encouraging results.
- Lymphoid radiotherapy (exploratory): encouraging preliminary results but still low level of evidence.
- Lung transplantation: last resort option in terminal cases, including retransplantation.
Prognosis and progression
The prognosis depends heavily on the etiology, severity at diagnosis, and response to treatment.
- PIBO in children: more favorable prognosis than post-transplant forms. Low mortality but high chronicity. Approximately 68% of children have a favorable outcome. In rare cases, partial resolution may occur. Forms associated with Stevens-Johnson syndrome are often progressive.
- Post-lung transplant BOS: poorer prognosis. The probability of remaining free of BOS at 5 years is only 36%. Post-BOS survival is approximately 51% at 3 years. The risk of death is approximately 6 times higher.
- BO associated with autoimmune diseases: immunosuppression can stabilize the clinical condition. Variable progression.
- Toxic BO: often stabilizes after exposure ceases, but does not generally regress.
Without treatment, the natural progression tends towards progressive chronic respiratory failure, which can be fatal.
Prevention: how to reduce the risks
- Up-to-date vaccinations: annual flu shot, pneumococcal vaccine, RSV immunoprophylaxis (palivizumab) for at-risk infants.
- Prompt treatment of respiratory infections: particularly in children, to limit bronchiolar damage.
- Respiratory protection in the workplace: appropriate equipment when exposed to volatile chemicals.
- Stop smoking and avoid passive smoking: a major aggravating factor.
- Close post-transplant monitoring: regular spirometry and prophylactic treatment with azithromycin.
- Caution with vaping: choose e-liquids certified as free of diacetyl and suspicious substitutes.
- Avoid any infectious contact: particularly for immunocompromised or transplant patients.
Research prospects and recent advances
Early biomarkers: identifying biological markers that enable diagnosis before fibrosis sets in is a major challenge. The cytokines IL-8 and IFN-γ, as well as serum LDH, are elevated in post-adenoviral forms and are the subject of predictive studies.
Lung microbiome: Studies on post-transplant SOB have shown that microbial dysbiosis is associated with an increased risk of BO and a more unfavorable outcome.
2023 Chinese international consensus: China has published a reformulation of the expert consensus on the diagnosis and treatment of BO in children, incorporating recent advances in early diagnosis and therapeutic strategies.
ERS/EBMT 2025 roadmap: An international working group has published a roadmap to improve early detection of post-allogeneic transplant BO, with proposals to redefine diagnostic criteria.
Predictive models and nomograms: Clinical nomograms can be used to predict the prognosis of POBO at the time of diagnosis, based on initial lung function and signs of bronchiolar inflammation.
Frequently asked questions (FAQ)
What is bronchiolitis obliterans in simple terms?
It is a disease in which the smallest airways in the lungs (the bronchioles) become inflamed, scarred, and gradually blocked. Airflow becomes increasingly difficult, causing chronic shortness of breath. Unfortunately, the damage is irreversible in most cases.
What are the main causes?
The four main causes are: severe respiratory infections (especially adenovirus in children), organ transplants (lung, bone marrow), inhalation of toxic substances (diacetyl, industrial chemical gases), and certain autoimmune diseases (rheumatoid arthritis, lupus).
Is bronchiolitis obliterans curable?
No, it is an irreversible disease. Treatments (corticosteroids, azithromycin, immunosuppressants, oxygen therapy) aim to slow its progression and relieve symptoms. In the most severe cases, a lung transplant may be considered.
What is the link between vaping and popcorn lung?
Diacetyl, a flavoring agent that gives a buttery taste, has been detected in some e-liquids. It is known to cause BO in workers who are heavily exposed to it. However, no formal cases of BO directly caused by vaping have been confirmed on a large scale. In Europe, most manufacturers have removed diacetyl from their products.
What is the difference between this and bronchiolitis in infants?
Acute bronchiolitis in infants is a common viral infection (often RSV), which is usually mild and resolves within a few weeks. Bronchiolitis obliterans is a rare and serious chronic disease that causes permanent damage to the lungs. These are two very different conditions despite their similar names.
How is bronchiolitis obliterans diagnosed?
The diagnosis is based on a combination of a compatible history, respiratory function tests showing fixed, irreversible obstruction, a high-resolution chest CT scan (mosaic pattern, air trapping), and sometimes a lung biopsy.
Can bronchiolitis obliterans be prevented?
Certain measures reduce the risk: up-to-date vaccinations (influenza, pneumococcus, RSV), prompt treatment of respiratory infections in children, occupational respiratory protection, smoking cessation, regular post-transplant monitoring, and caution with flavored e-liquids.
Sources and references
- StatPearls / NCBI — Bronchiolitis Obliterans
- Orphanet — Bronchiolitis obliterans (ORPHA:1303)
- ISHLT/ATS/ERS — Diagnosis and Management of BOS (2014)
- RespiRare — Bronchiolitis obliterans not related to transplantation
- Quebec Lung Association
- Frontiers in Pediatrics — Risk Factors for PIBO/Adenovirus (2024)
- Canadian Respiratory Journal — Postinfectious BO in Children (2025)
- Canadian Respiratory Journal — PIBO Workshop Report (2020)
- European Lung Foundation — Treatment of pulmonary cGvHD
- National Jewish Health — Bronchiolitis Obliterans
Disclaimer: This article is provided for informational and educational purposes only. It is not a substitute for medical advice. If you or your child have persistent respiratory symptoms, consult a doctor or pulmonologist.